With well over one million infections and nearly 7,000 deaths, the Omicron variant has dealt Hong Kong its heaviest blow since Covid-19 emerged as a worldwide threat some two years ago, after earlier outbreaks in the city were successfully stemmed.
The epidemic as well as the government’s draconian restrictions put major stress on many institutions in the city, from public hospitals, to shops, schools, businesses, and mortuaries. So how did public institutions and millions of Hongkongers react to and cope with this deadly wave? HKFP examines how Omicron’s impact on the city was felt, in eight data charts.

Hong Kong recorded its first local Omicron case on New Year’s Eve, almost three months ago. Some 4.6 million or about 62 per cent of the city’s 7.4 million people had been given two doses of vaccine at the time. Vaccines were not made available to children under 12 until late January, and crucially only about 20 per cent of those aged 80 and above had been jabbed.
Despite the government’s urging and restrictions on the unvaccinated, some saw little incentive to get jabbed when the city had been almost Covid-free for eight consecutive months.
Vaccinations
As the fifth wave worsened in January, however, those who were previously vaccine-hesitant began to change their minds. Among those who got their first dose in the fifth wave, nearly a million people – about 62 per cent – opted for Sinovac instead of BioNTech. The rush for the first dose of Sinovac was most apparent in the second week of February, while the rush for the second dose came only when infections hit their peak on about March 3, with close to 80,000 positive cases a day.
However, for those who had been fully vaccinated with two doses even before the fifth wave hit, the trend was reversed. About 67 per cent of them chose BioNTech for their third booster dose.
Internet self-help
As it became clear by the end of February that the outbreak was out of control, with tens of thousands infected every day, many turned to the internet for help. Google Trends data – which reflects the popularity of a topic queried by Hong Kong users irrespective of language – showed the number of searches on sore throat and fever started increasing about two to three days before the number of infections did.

A group of British medical researchers compared Google Trends data on queries about loss of taste and of smell to the number of Covid-19 infections as early as April 2020. Despite anecdotal reports, these symptoms had yet to be established as caused by Covid-19, because attention was paid mostly to more severe symptoms such as fever or coughing. Based on their remarkable correlation, researchers moved closer to identifying a previously unknown symptom.
After identifying their Covid-19 symptoms, Hongkongers searched the internet for medication. Searches for medication to suppress fevers – paracetamol and the branded drug Panadol – visibly increased.
But the biggest surge in queries was for Lianhua Qingwen, an over-the-counter traditional Chinese medicine for symptoms including sore throat and fever. The search peaked on the same day as the number of infections. Searches for the shortened term “lianhua,” which means lotus, also spiked at the same time. It was around this period when many pharmacies reported a shortage of Panadol due to a sudden surge in demand.
Overcrowded hospitals
What Omicron lacked in severity, it made up for in infectiousness. While most patients experienced symptoms mild enough to be treated at home using over-the-counter medication, the exponential rise in numbers meant those in serious condition – especially the elderly – began to overwhelm hospitals.
General in-patient bed occupancy at public hospitals exceeded 100 per cent by about mid-March, with hundreds crammed in corridors and lift lobbies. Patients overflowed outside emergency rooms from early February, when hospitals had no free beds.
To cope with patients awaiting admission, hospitals such as the Caritas Medical Centre and Queen Elizabeth Hospital erected tents outdoors. Harrowing images of elderly patients in beds exposed to the chilly weather captured the human cost of Hong Kong’s spiralling fifth wave.

Ambulance services were stretched thin even before the number of infections began its unimaginable climb. Before the city allowed home isolation and opened temporary isolation facilities comprised of converted cargo containers, patients’ sole resort was to seek isolation and treatment at a public hospital.
In early February, as reports emerged that patients waited for days before they could be picked up by an ambulance, a Hospital Authority (HA) official said they should take taxis to a public hospital. He reversed his position two days later, urging those with mild symptoms not to go to hospital.
In late February, of almost 2,000 emergency calls received daily , the Fire Service Department’s ambulances were able to reach patients within 12 minutes – its target response time – only about 20 to 30 per cent of the time. The government later introduced dedicated taxi and bus fleets to shuttle Covid patients to government clinics, easing the burden on emergency services.
Sick medics
Doctors, nurses and other hospital staff who worked tirelessly to provide care were themselves vulnerable. Over 20 per cent of the HA’s 88,000 staff contracted Covid-19 at one point during the fifth wave, leaving services more overstretched than ever. As of Friday, 4,300 remained out on Covid-19 sick leave.
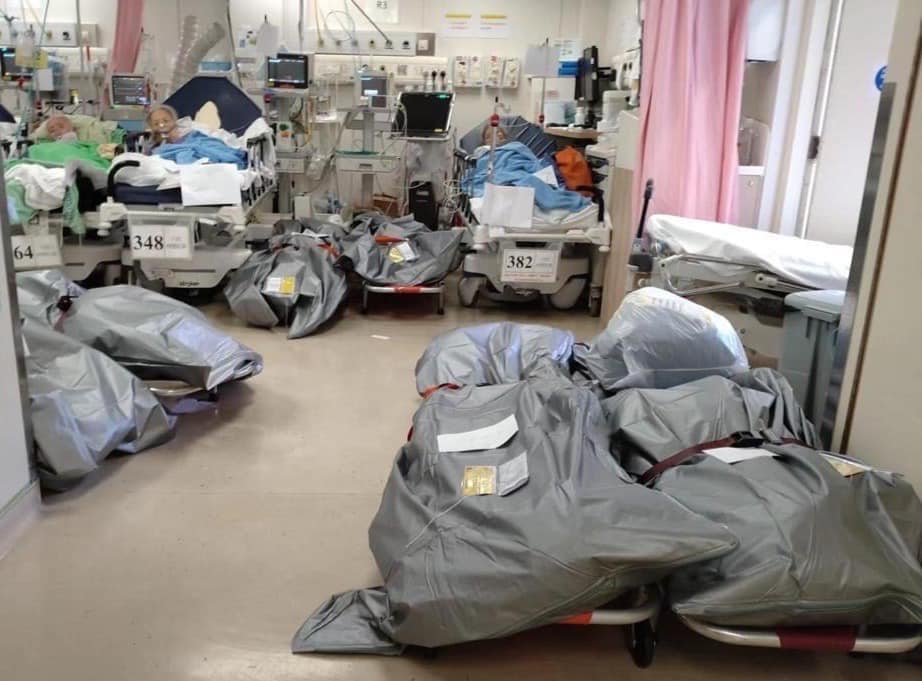
Death toll
The ultimate toll of an epidemic is the lives it claims. A photo taken at Queen Elizabeth Hospital in early March showed body bags left on stretchers next to patients in a ward.
Public mortuaries managed by the Department of Health had a normal capacity of 646 bodies, which could be stretched to about 1,070 using all storage compartments including mobile units. After adding some 50 refrigerated containers, capacity increased to 3,745 on March 17, according to a tally compiled by HKFP based on past government figures and releases.

Neither the HA nor the Department of Health provided mortuary storage statistics despite HKFP’s request. With its 3,000-odd hospital mortuary compartments in total, the HA said it faced “immense pressure” and had reached “full capacity.” The DH only supplied the number of bodies in storage at the city’s four public mortuaries on two dates.
Support HKFP | Policies & Ethics | Error/typo? | Contact Us | Newsletter | Transparency & Annual Report | Apps
Help safeguard press freedom & keep HKFP free for all readers by supporting our team

LATEST ON COVID-19 IN HONG KONG
HKFP GUIDES
Support HKFP | Policies & Ethics | Error/typo? | Contact Us | Newsletter | Transparency & Annual Report | Apps
Help safeguard press freedom & keep HKFP free for all readers by supporting our team